Osteoarthritis in cats is a pathology that is rarely diagnosed but which is very frequent.
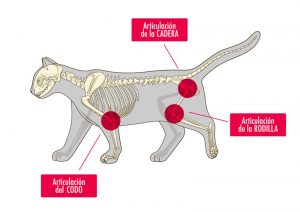
About 40 % of cats over 7 years of age have signs of osteoarthritis in some joint, among which the lumbosacral and coxofemoral joints, the elbow and the knee are the most affected ones.
The reason why it is not diagnosed in many cases is probably that cats suffering from osteoarthritis do not limp or show any change in their way of walking in any objective way, signs that in other species, such as the dog, would lead the pet owner or the veterinarian to the joint pathology.
The cat that is suffering from osteoarthritis stops climbing to high spots, doubts before jumping, rejects being brushed, does not want to be picked up and, in general, is more irascible. The diagnosis of this pathology is performed by means of simple radiography, and the clinical signs and symptoms of the patient always have to be related to the radiologic findings: cats with clear sympthoms of joint pain may show minor radiologic signs, and viceversa, patients with very severe radiologic signs lead a normal life.
The use of meloxicam is recommended to control joint pain in cats, which in this species is authorized to be used as maintenance drug for this pathology.
When meloxivet is needed for a period of time remember it can also be used at lower doses such as 0.02 -0.05 mg/kg and it can be combined with tramadol drops or tablets because using these doses it can also be used in patients with renal pathologies.
These patients should be carefully monitored for obesity, since excess weight on joints magnifies pain and worsens the progression of osteoarthritis.
Chondroprotectors
They are drugs that contain cartilage precursor substances, and they are used as a complement in the tratment of osteoarthritis together with NSAIDs, mainly when there is not acute crisis of the disease. They are known as disease-modifying substances and they are considered dietary supplements.
Its mechanism of action consists in providing the elements that are reduced in osteoarthritis, since there exists a deficiency in cartilage repair capacity.
A beneficial effect on the joint may be observed, either by stimulation of proteoglycan and collagen synthesis by chondrocytes, by means of an anti-inflammatory activity or by an antithrombotic fibrinolytic activity.
Among the most commonly found compounds we can mention:
- Hyaluronic acid: This is an important compound of the synovial fluid, it is administered intra-articularly and it protects cartilage since it lubricates joints and inhibits diapedesis of white blood cells in the joint.
- Glycosaminoglycan polysulfate: this compound binds to connective tissue due to the high negative charge of its sulphate groups.
- Chondroitin sulfate: It is a glycosaminoglycan that is extracted from cartilage, it is administered orally. This condroprotector inhibits the enzymes that degrade cartilage, it has the capacity to stimulate the synthesis of glycosamines and collagen, and it inhibits inflammation. The product is well tolerated and there are no toxicity reports.
Glucosamine: It stimulates hyaluronic acid, proteoglycan and collagen synthesis by chondrocites. It also stimulates the synthesis of anti-inflammatory fibroblasts independent from the cyclooxygenase.
Conclusions:
NSAIDs provide a quick resolution to pain and inflammation but, generally, once they are suspended, they show a progressive regression to the initial clinical features, because they are not capable of modifying the natural course of the disease.
In some studies, Chondroprotectors showed a favorable response, although it could be slow, and these effects lasted longer after the treatment was suspended but they did not disappear.
It should be remembered that, to date, there is no drug that provides the patient with complete healing or total recovery from degenerative joint disease; in spite of advances, even surgical advances such as total replacement or even arthroscopy, since it is not posible to say that any treatment is 100 % effective.

